Home » World News »
Improve ventilation and make antiviral drug widely available, long COVID inquiry hears
GPs say they are unable to properly care for the hundreds of thousands of Australians with long COVID due to outdated Medicare rules, and a leading scientist has called for wider access to a drug that potentially prevents the disease.
At a federal parliamentary inquiry into long COVID on Monday, experts said patients with the disease often had a wide range of symptoms that needed complex, careful management, not just from a GP but also a team of specialists – including physiotherapists and psychologists.
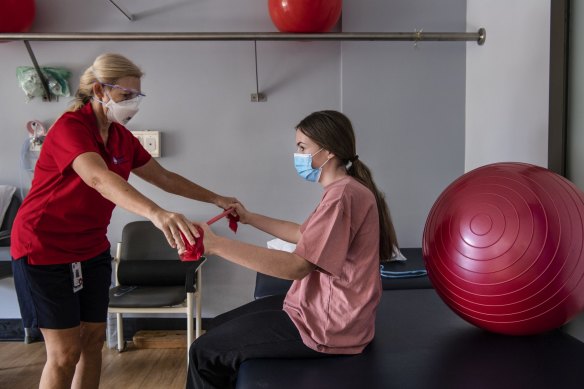
Payton Jacobs, 18, with physiotherapist Anne Tanner at NSW’s first long COVID clinic.Credit:Louise Kennerley
Medicare subsidises only five allied health sessions a year, which can go within a couple of weeks if a patient needs to see different experts.
“They don’t really provide adequate support,” Professor Mark Morgan, a Royal College of GPs spokesman, told the inquiry.
Subsidised sessions for chronic illness care kick in only if a person’s illness is likely to last longer than six months, which is not always the case for people with long COVID. Waiting for the disease to become chronic meant doctors missed an opportunity to intervene early, Morgan said.
Current Medicare rebates penalise GPs for longer consultations. “It’s clearly insufficient,” Morgan said.
Deakin University modelling estimates the number of Australians with long COVID is between 160,000 and 1.2 million, with between 35,000 and 196,000 severe cases.
There are no proven treatments for long COVID nor methods to prevent it, other than avoiding infection in the first place, the inquiry heard.
But one drug has shown promise: the antiviral medicine Paxlovid, which is used to protect the vulnerable when they fall ill with COVID-19.
A large study looking at 9217 people with COVID being treated with Paxlovid found the drug cut the risk of developing long COVID by 26 per cent. The study has not yet been published in a peer-reviewed journal.
While noting it wasn’t a cure, director of the Burnet Institute Professor Brendan Crabb said he would privately purchase Paxlovid if he were diagnosed with COVID-19. The drug should be available to anyone diagnosed with COVID, he said.
“I’m very much in favour of much wider availability of antivirals,” he said. “If I was diagnosed, I would spend $1000 on that drug. I’m not waiting for severity – I will have it.”
Crabb said the most important thing the inquiry could do was recommend long COVID be taken seriously by the federal government. Without a sense of national prioritisation, he said, “it’s very hard for employers to take it seriously … it’s difficult for a lot of health professionals to take it seriously”.
Brain fog, one of the disease’s hallmark symptoms, perfectly illustrated the issue by making the condition sound like it was all in your head, Crabb said. “It’s actually brain damage,” he said.
The focus of much of Monday’s hearing was on measures to improve ventilation and prevent airborne transmission of COVID-19.
Government MP and inquiry member Dr Michelle Ananda-Rajah told the committee mandatory indoor air quality standards needed to be developed.
Monday also marked the start of wider availability for a fifth COVID-19 vaccine dose. All adults are eligible if it has been six months since their last vaccination.
The Health Department hopes the rollout will help address the country’s falling booster rates: just 44.8 per cent of eligible adults have had a fourth dose.
Dr Lucas de Toca, head of the department’s primary care response to COVID-19, told the inquiry on Friday: “There is no catch-up. There is no counting of numbers. We need to start to move the narrative away from those numbers.”
Liam Mannix’s Examine newsletter explains and analyses science with a rigorous focus on the evidence. Sign up to get it each week.
Most Viewed in National
From our partners
Source: Read Full Article