Home » World News »
Common anti-anxiety meds turning Australians into accidental addicts
Save articles for later
Add articles to your saved list and come back to them any time.
Common anti-anxiety drugs such as Valium and Xanax are being prescribed for dangerous lengths of time, experts have warned, resulting in people developing addictions. Some 1.4 million Australians were prescribed 5.1 million scripts of benzodiazepine anxiety medications in 2020-21.
The medications are the second-most common drug involved in accidental overdose deaths behind opioids, according to the Penington Institute’s Annual Overdose Report. The proportion of accidental overdose deaths due to benzodiazepines has doubled in the past 20 years, up to 32.5 per cent in 2021.
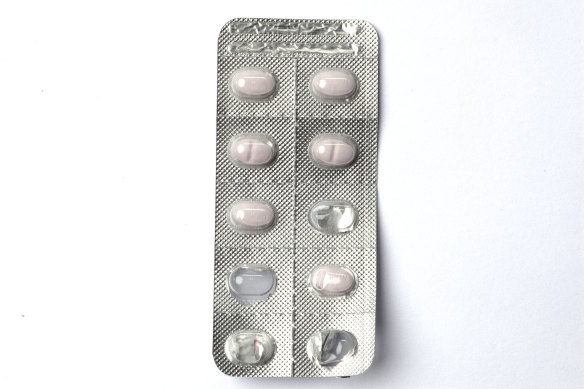
Xanax and Valium are common benzodiazepines used to treat anxiety. Credit: Jennifer Soo
The National Prescribing Service and the drug manufacturers themselves recommend benzodiazepines only be prescribed for a maximum of four weeks.
Janet Shaw, who runs the country’s only specialist benzodiazepine treatment centre in Melbourne said the risk of benzodiazepines is not explained to patients.
“Clients generally have been taking legitimate medication that the doctor has prescribed for them for an inappropriately long period of time,” she said. “We have clients who have been taking benzodiazepines for 50 years.”
Most don’t realise they are dependent until they see a different healthcare provider who alerts them to it until they skip a few doses or see coverage of the dangers in the media.
“They absolutely don’t see themselves as a drug addict or addicted or needing a drug service at all,” Shaw said.
Shaw said coming off benzodiazepines is not easy as they can have worse withdrawal symptoms than heroin or ice, causing delusions, hallucinations, psychosis, seizures, suicidal thoughts and heart palpitations.
University of Sydney School of Pharmacy associate professor Danijela Gnjidic said benzodiazepines should be under similar scrutiny to opioids.
“Benzodiazepines are similar to opioids as they’re a central nervous system drug, are very hard to stop and taper, and many patients are more likely to be caused harm by them than benefit from them, especially with long-term use,” she said.
In 2016, the government introduced a raft of measures to limit opioid-related deaths including smaller pack sizes to limit unused tablets, warning labels on packaging, and guidelines for medical professionals to stop or reduce opioids from the moment they’re prescribed.
Gnjidic, who developed the guidelines, believed Australia needed similar directions for benzodiazepines, which Canada has already implemented.
“Long-term use is quite commonly observed, and it’s particularly problematic if they’re co-prescribed with other high-risk medicines [such as antipsychotics],” she said.
A spokesperson for Health Minister Mark Butler referred questions to the Therapeutic Goods Administration.
“The potential risks of benzodiazepines are well-known,” a TGA spokesperson said, adding warnings are included in drug information material advising prescribers to exercise caution in prescribing benzodiazepines to people at risk or with a history of hazardous or harmful use.
“Benzodiazepines are an important treatment for a range of conditions and can be used safely when prescribed in accordance with relevant clinical guidelines. When used appropriately, the benefits of using these medicines outweigh the potential risks.”
Natalie had no idea she had developed a dependency on the anti-anxiety medication prescribed by her doctor.
Prescribed Valium for anxiety by her psychiatrist in 2014, Natalie – who asked for her surname to be withheld to protect her privacy – took a tablet a day and followed the direction of her healthcare provider.
Coming off benzodiazepines is not easy as they can have worse withdrawal symptoms than heroin or ice.Credit: Rob Banks
She was prescribed additional and increased dosages of the drugs for four years as her anxiety worsened, taking Clonazepam and Alprazolam daily.
“I remember being sceptical, but I took it because I felt desperate, and no real risks were articulated to me,” she said.
Natalie’s mental health worsened, resulting in a stay at the psychiatric hospital, where doctors started tapering her off the drugs. She suffered severe withdrawal symptoms.
“It was really, really intense,” Natalie said of the withdrawals, which consisted of vertigo, disorientation, mood swings and suicidal thoughts. After two years of slowly tapering, Natalie is now off benzodiazepines but still experiences brain fog and issues with balance.
“Had I known what I know now, I wouldn’t have touched it,” she said.
Start the day with a summary of the day’s most important and interesting stories, analysis and insights. Sign up for our Morning Edition newsletter.
Most Viewed in National
From our partners
Source: Read Full Article